Hypospadias
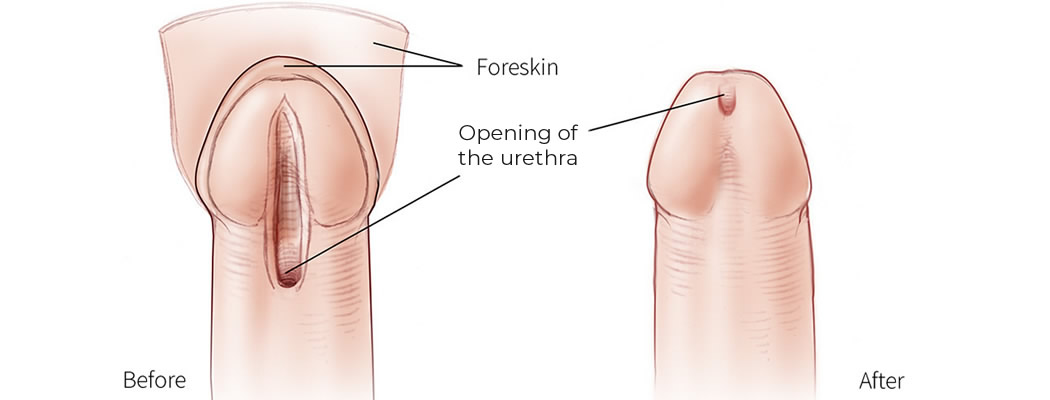
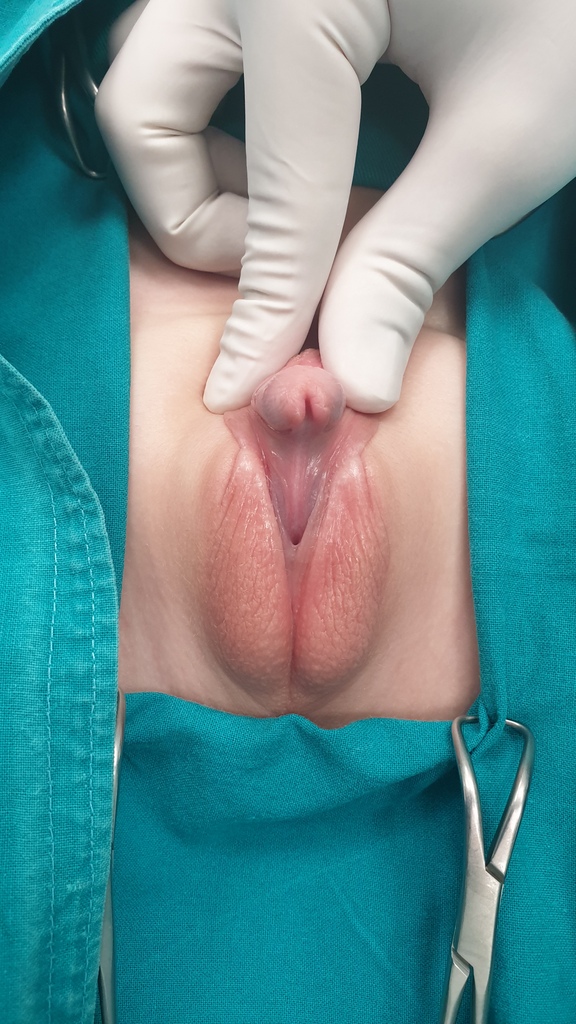
Hypospadias is a common congenital anomaly of penis with an abnormal opening of the urethral meatus on the underside of the penis. The anomaly is also characterized by hooded foreskin and downward curved penis. Often, other congenital malformations such as undescended testicles and inguinal hernia can be seen.
What are the causes and risk factors for hypospadias?
The exact cause of hypospadias is unknown. It can be seen in one in 250 newborn boys. The exact cause of hypospadias has not yet been discovered. The most likely cause of hypospadias is hormonal imbalance during fetal development. Recently, there has been an increase in the number of patients with hypospadias in developed countries of the world.
Risk factors are:
- exposure to certain substances during pregnancy (hormones, pesticides or industrial chemicals)
- family history
- maternal age over 35
- low birth weight babies.
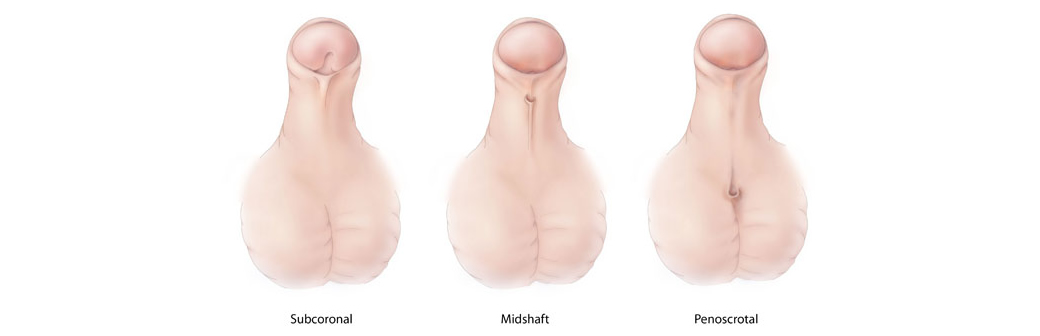
Classification of hypospadias?
The classification depends on the location of the urethral opening and the curvature of the penis. The greater the distance of the urethral opening from the tip of the penis, the more severe the disorder. Related to severity hypospadias are classified into:
- mild hypospadias (urethral opening is localized at midshaft of the penis or within the head of the penis, without curved penis)
- moderate hypospadias (urethral opening is localized on the midshaft of the penis, there is moderate curvature of the penis)
- severe hypospadias (urethral opening is localized at the base of the penis, scrotum, or beneath the scrotum, with associated curved penis).
How to diagnose hypospadias?
The diagnosis of most hypospadias is made by physical examination at child birth by pediatrition, but slight displacement of the urethral opening may be subtle and difficult to identify. When diagnosis is made childe will be refered to a pediatric urologist who is specialized in genital reconstrutive surgery.
If there are other malformations present, the psychical examination is not enough. Other diagnostic procedures should be done.
Severe hypospadias with unilaterally or bilaterally non-palpable testis or ambiguous genitalia requires a genetic and endocrine assessment performed by experienced multidisciplinary team to exclude possible disorder of sex development (DSD), congenital conditions with atypical development of chromosomal, gonadal or anatomical sex.
How do you treat hypospadias?
The treatment of hypospadias is surgical. The age at surgery is usually 6-18 months.
Two months before surgery topical hormonal treatment with di-hydro-testosterone (Andractim©) needs to be conducted. Local hormonal treatment leads to enlargement of the glans and shaft of the penis.
After conducted a local treatment an adequate sized neo-urethra with opening on the glans needs to be formed with proper skin coverage of the penis. The penile curvature must be corrected. The shorter the urethra and the more curved the penis, the more difficult it is to correct hypospadias with surgery.
Most forms of hypospadias can be corrected in a single surgery, but sometimes there is need for more than one surgery.
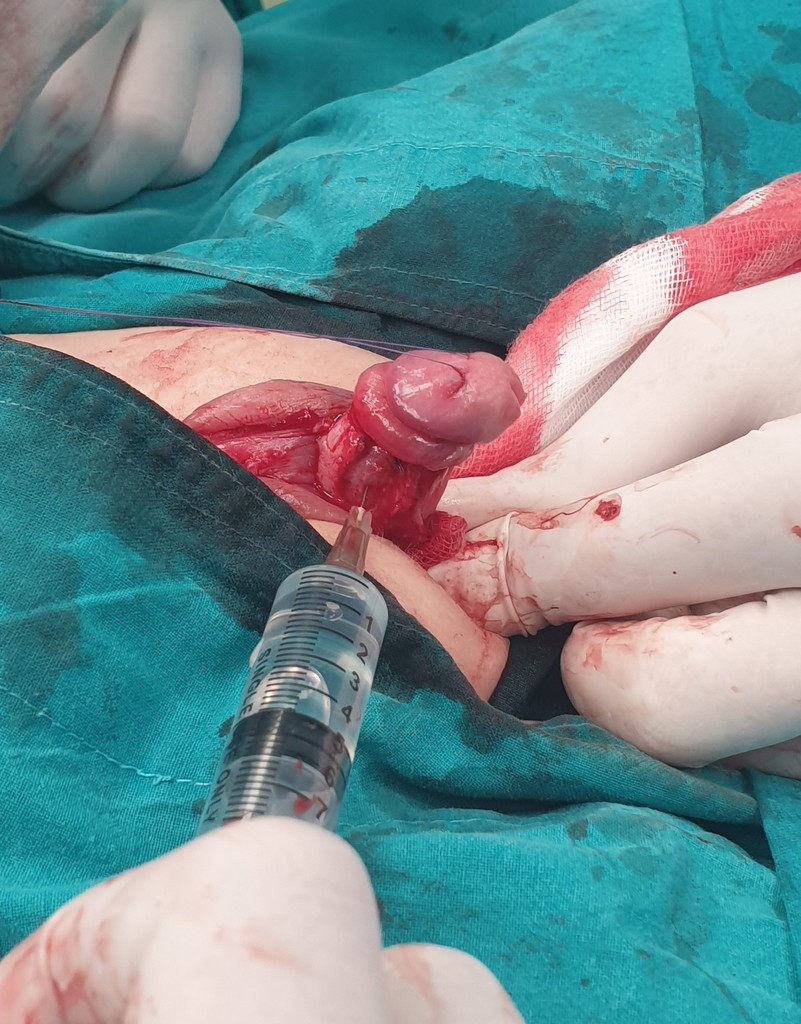
Hypospadias repair surgery
The child is put the child is put under (general anesthesia) for this surgery. The child needs to be healthy before surgery to avoid the risk of anesthesia-related complications.
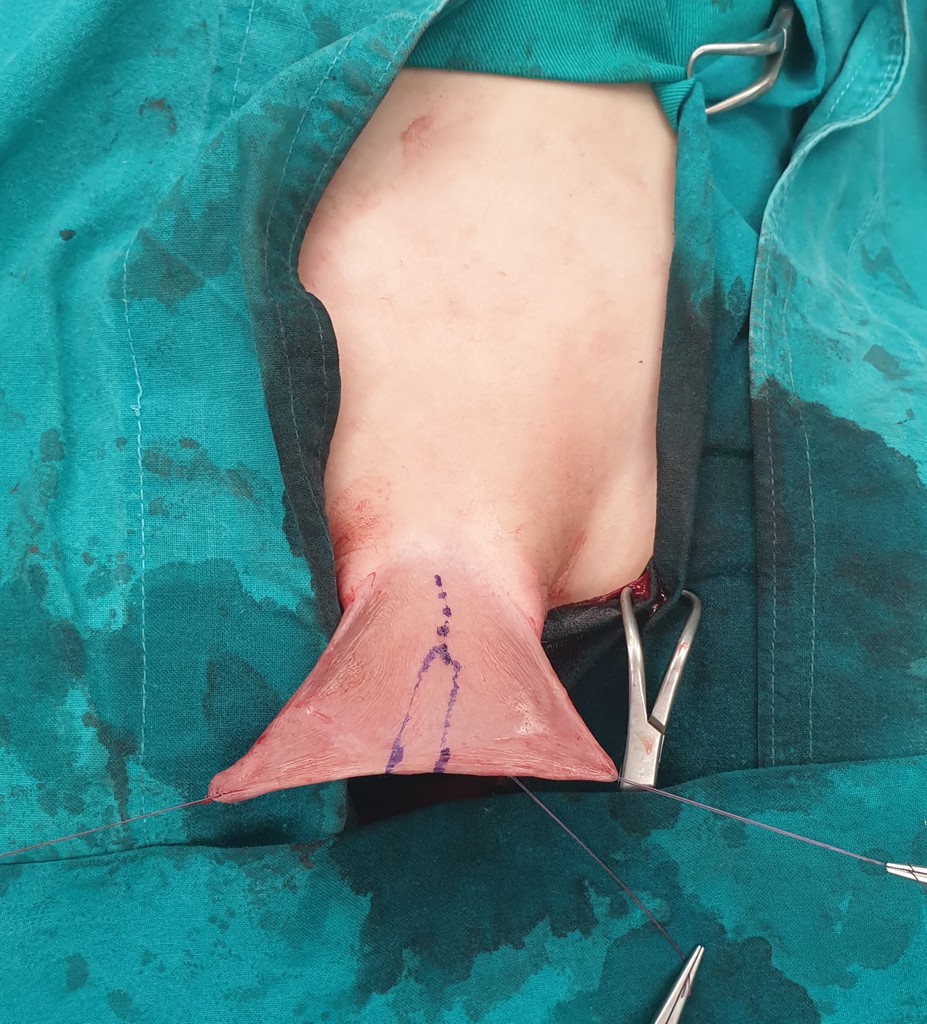
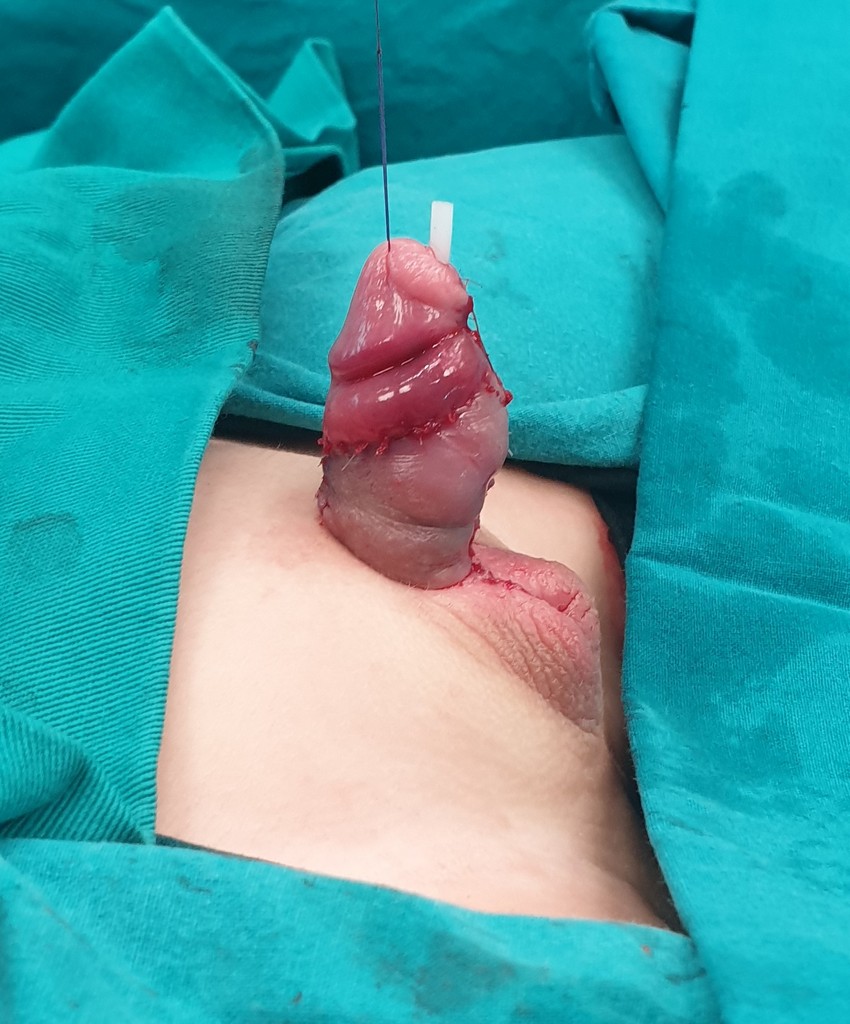
An adequate sized neo-urethra with opening on the glans needs to be formed with proper skin coverage of the penis. The surgeon may need to use tissue grafts from the foreskin or from the inside of the mouth (buccal mucosa graft). The decision to choose the surgical technique that will be used to form the urethra is often made during the operation itself, and therefore the surgeon needs to be experienced. The curvature needs to be corrected also. After moving the blood vessels and nerves, the curvature is being corrected. This is followed by the creation of a normal, conical shaped glans and the formation of a new urethral opening at the top of the glans. The operation ends with reconstruction of the skin of the penis and placement of a compressive bandage. Urine is drained with a suprapubic tube so that the wounds on the penis can heal properly. Stitches that dissolve on their own will be placed. The surgery for mild types can take an 1-2 hours, but for severe types it can take up to 3 hours.
What are the possible complications after surgery?
Fistulas are the most common postoperative complications. They represent abnormal communication between the skin on one side and the urethra on the other and they require surgical intervention to remove them. In addition, wound infections and separations of suture lines are possible. However, with modern surgical techniques, complications are minimal.
Follow up after surgery
Hospital stay after surgery depends on the age of the patinet and the severity of the hypospadias. Most patients can go home after one night spent in the hospital. Prophylactic antibiotics are given as well as the medication for pain. The first dressing change is after two days. Urethral stent and compression dressing are usually removed by seventh postoperative day and after three days suprapubic tube is removed if child is voiding normally.
Periodic monitoring of these patients is necessary until sexual maturity is established and adequate sexual function of the penis is confirmed. After successful surgical treatment, penile growth continues and the function of the penis is preserved and normal.